What Is Vesicular Athlete’s Foot?
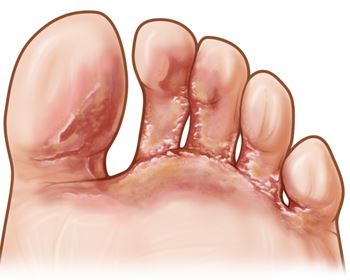
Vesicular Athlete’s Foot is a fungal infection occurring on the skin. The onset of the disease is usually marked by a sudden outbreak of fluid-filled areas in the skin. In most cases, the blisters develop on the skin of the instep but are sometimes found between the toes, sole or top of the foot, and in the heels.
Causes
Vesicular athlete’s foot is caused by a fungal infection. The fungi responsible for this disease is well adapted to live and feed on the skin protein known as keratin. This fungus thrives in tropical climates, especially where temperatures are above the roof.
That said, it means that wearing of tight, non-breathing footwear paves the way for the growth and development of the fungi that causes the infection.
These fungal organisms can be passed from one person to another through sharing bathrooms, gym locker rooms, and swimming pools. Blisters and cuts on the feet make it easier for the fungi to cause vesicular athlete’s foot infection.
It is believed that the vesicular athlete’s foot is as a result of the allergic reaction of the body against fungal organisms. This response subsequently leads to the formation of blisters in the affected regions. Ulcerative tinea pedis is a severe case that affects large areas and is usually accompanied by bacterial infections on top of the fungal infection.
Signs & symptoms
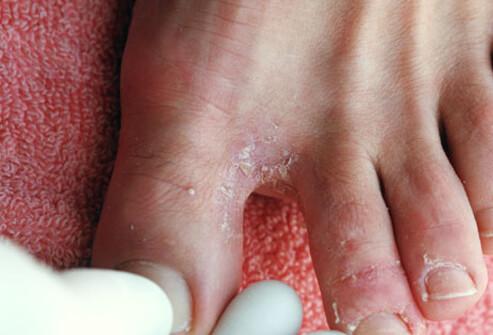
Athlete’s foot typically occurs between the fifth and fourth toes or between the fourth and third toes. Their onset is accompanied by persistent itching and scaling of the affected areas leading to cracked and soggy white toes.
The infection can be transmitted to the sole of the feet. The condition may worsen if you frequently wear tight socks or shoes that increase moisture in your toes. If a bacterial infection also sets in, the surrounding skin will ooze off, burn, and produce an awful smell.
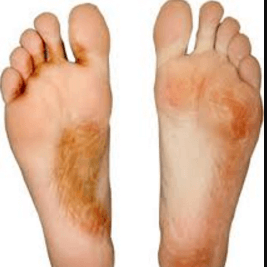
On the contrary, the moccasin-type infection does not cause inflammation or the itchy feeling. Instead, it causes the entire sole and heel region to become dry and flaky with the resultant scales forming moccasin-like patterns. In some instances, the infection may spread to the toenails, and this becomes a complication that has proven difficult to treat.
People suffering from a vesicular-type infection have sore, fluid-filled blisters located between the arch sides of the foot and the toes. These blisters are due to the allergic response of the body to the fungi causing athlete’s foot.
The most common type of athlete’s foot infection is the interdigital tinea pedis which is presented in the form of a softened tissue arising due to soaking. It is also characterized by the presence of scales in the web spaces between the toes. In the case of a secondary bacterial infection, ulceration, which is marked by painful ulcers between the toes and is hard to treat, may occur.
Tinea pedis can lead to an infection of the foot referred to as cellulitis. This can be particularly worrying to individuals diagnosed with vascular chronic disease or diabetes.
Diagnosis
Doctors can easily diagnose athlete’s foot by examining your feet for itchiness, scaling, and strong odors. The doctors or practitioners can further confirm the infection and isolate it from other skin diseases such as ringworm, eczema, and psoriasis by collecting a sample of the lesions and sending them to the lab for testing.
Treatment
When the infection progresses and starts appearing as soggy, inflamed blisters with foul smell, medical advice is highly recommended. Where a secondary bacterial infection is in play, the doctor will first prescribe medication for the bacteria before using antifungals on the primary fungal infection.
Over-the-counter prescription or tropical antifungals such as gel, solutions, creams, and lotions offer the best medication option for uncomplicated cases of athlete’s foot. In case they are not effective, antifungal pills are prescribed.
Some medications contain both antibacterial and antifungal ingredients to assist in speeding the healing process. Also, dressings using aluminum acetate -treated clothes may be useful when applied to macerated or vesiculated lesions. Shoes can also be treated using antifungal powders.
A foot infection that doesn’t go away even after appropriate treatment has been applied for fungal and bacterial infection implies another infection other than athlete’s foot. The symptoms may be caused by a different skin disease necessitating the need to see a doctor for treatment regularly.
Prevention
Foot care
Taking good care of your feet is the surest way of preventing athlete’s foot. Proper care can be manifested in the following ways:
- Keep your feet clean, dry and fresh.
- Wear sandals or shoes that allow your feet to breath or “air out.”
- Always remember to dry the region between your toes after bathing or swimming.
- Allow your shoes to air out for a minimum of 24 hours before wearing them again
- Change your socks on a daily basis.
- Avoid tight-fitting shoes and footwear.
- Wear soft socks to absorb sweat.
- Use talcum or antifungal powders.
- When indoors, remove your shoes.
- Wear shower sandal when in public showers or pools.
If you detect symptoms of athlete’s foot in your feet, make sure to dry the groin area before and after bathing. Also, put on your socks before putting on your innerwear.
This prevents the spreading of the infection from the feet to the groin that results in jock itch.
You may choose not to treat athlete’s foot if there are no severe symptoms or the symptoms don’t disrupt you from your daily routine.
However, if you have a condition that may increase the rate of infection such as diabetes, then, the best alternative is to see a doctor.
In some cases, athlete’s foot infection may lead to cracks and blisters that open up the body to bacterial and fungal infections. If such infections are left untreated, they can quickly spread to other people.
In a nutshell, the best prevention method against athlete’s foot is good hygiene. This entails keeping the feet cool and dry.
Pictures
References
- Crawford F (2009). Athlete’s foot, search date July 2008. Online version of BMJ Clinical Evidence: http://www.clinicalevidence.com.
- Murray MT, Pizzorno JE Jr (2006). Melaleuca alternifolia (Tea Tree). In JE Pizzorno Jr, MT Murray, eds., Textbook of Natural Medicine, vol. 1, chap. 104, pp. 1053–1056. St. Louis: Churchill Livingstone Elsevier.
